Gouty arthritis: spot symptoms and act fast
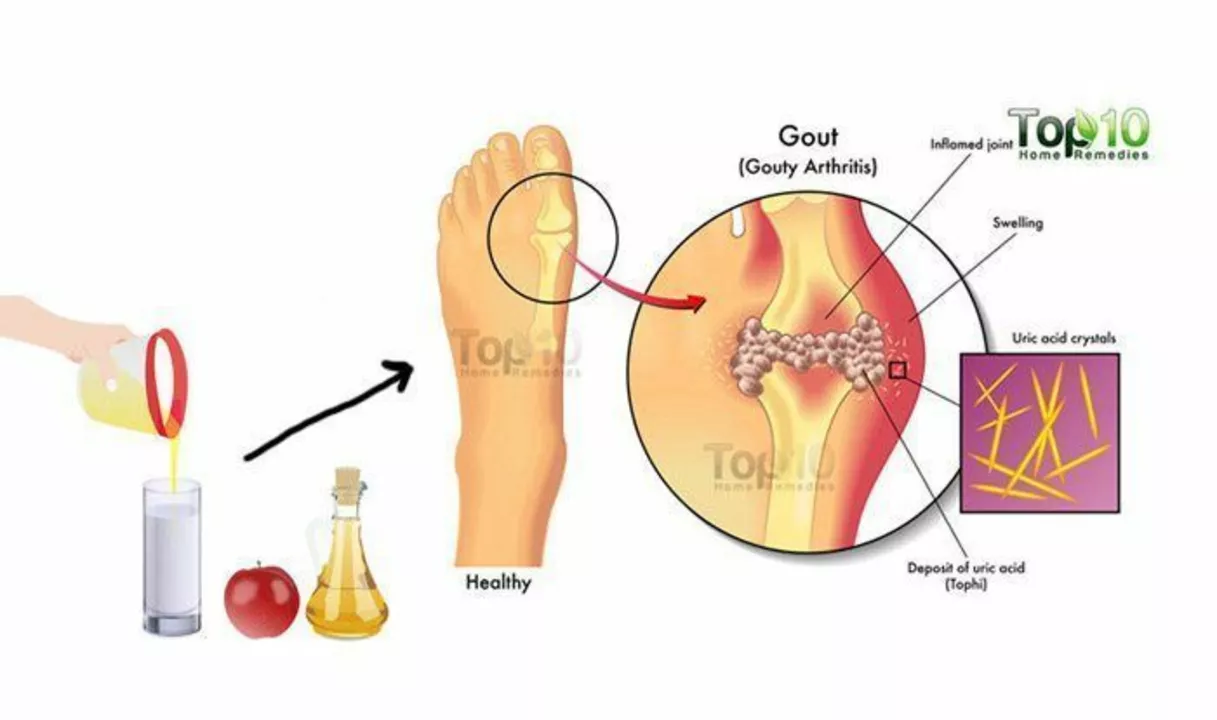
Ever wake up with your big toe on fire? That classic sudden, intense pain is often gouty arthritis. It’s caused by tiny monosodium urate crystals piling up in a joint. Those crystals spark sharp inflammation, swelling, redness and stiffness. Knowing the signs and what to do right away can keep a bad attack from turning into a long-term problem.
What causes gouty arthritis and how it’s diagnosed
Gout starts when uric acid—made when your body breaks down purines—builds up. High uric acid can come from the foods you eat (like red meat and shellfish), excess alcohol—especially beer—certain medicines, kidney problems, or family history. A single trigger, such as a big meal, dehydration, or surgery, can spark an attack.
Doctors diagnose gout by looking at symptoms and tests. Joint fluid analysis (looking for needle-shaped crystals) is the gold standard. Blood tests measure serum uric acid, but levels don’t always match symptoms, so they use both the lab results and the clinical picture. If you get recurrent attacks, imaging or specialist referral may follow.
Practical steps to manage attacks and prevent future ones
Short-term and long-term care are different. For an acute attack, fast pain relief matters: over-the-counter NSAIDs (like ibuprofen), prescription colchicine, or a short course of oral steroids work well when used as directed. Call your doctor before starting prescription meds—timing and dosing matter.
To lower the chance of future attacks, focus on predictable fixes:
- Cut high-purine foods: limit organ meats, anchovies, sardines, shellfish and large portions of red meat.
- Skip beer and reduce hard liquor; sugary sodas and fruit juices raise risk too.
- Drink water. Staying well-hydrated helps kidneys clear uric acid.
- Lose weight gradually if needed. Crash diets can trigger attacks.
- Choose low-fat dairy, whole grains, vegetables and cherries—these are linked to lower risk.
- Talk to your doctor about coffee and vitamin C—both can modestly lower uric acid for some people.
If attacks are frequent or you have tophi (lumpy deposits under the skin) or joint damage, urate-lowering therapy (ULT) like allopurinol or febuxostat may be recommended. The goal is usually to push serum uric acid below 6 mg/dL, but the target and timing should be set with your provider. Don’t start or stop ULT on your own—changes need medical oversight and often slow dose adjustments.
Living with gout is manageable when you know triggers and have a plan. Treat attacks early, use lifestyle changes to reduce uric acid, and work with your clinician on long-term therapy if attacks keep coming. If you’re unsure whether pain is gout, get checked—early diagnosis prevents lasting harm and helps you get back to normal faster.
The Role of Genetics in Gouty Arthritis: Are You at Risk?
As a blogger, I recently delved into the fascinating topic of genetics and its role in gouty arthritis. What I discovered is that genetics plays a significant part in determining an individual's risk for developing this painful condition. In fact, certain genes have been identified that are associated with an increased risk for gout. This means that if you have a family history of gout, you may be more susceptible to developing it yourself. It's crucial to be aware of this genetic link and take preventive measures to minimize your risk of experiencing the discomfort of gouty arthritis.
- Drug Information (75)
- Health and Wellness (60)
- Pharmacy Information (28)
- Medical Conditions (24)
- Supplements (5)
- Diabetes (4)
- Travel Health (3)
- Mental Health (3)
- Heart Health (2)
- Parenting (2)
-
Healthcare System Shortages: How Hospital and Clinic Staffing Crises Are Affecting Patient Care
1 Dec 2025 -
International ICH Guidelines: How Global Harmonization Improves Medication Safety
31 Dec 2025 -
Statins and Nonalcoholic Fatty Liver Disease: Safety, Benefits, and What to Monitor
3 Jan 2026 -
Lupus Arthritis and Hydroxychloroquine: How This Drug Reduces Joint Inflammation and Prevents Flares
1 Dec 2025 -
Buy Cheap Generic Lasix Online - Complete Guide
4 Oct 2025

2.06.23
Alistair Mukondiwa
11