Genetics: What Your Genes Mean for Medicine and Everyday Health
Genes aren’t just for family photos and eye color. They change how your body reacts to drugs, what risks you might have for certain diseases, and even how likely supplements or diets will help. On this page you’ll find clear, practical info about genetics and medicine — what matters now and what’s coming next.
Pharmacogenomics is the name for how genes affect drug response. A simple test can tell whether a medicine will be less effective or more likely to cause side effects for you. That matters for common drugs like antidepressants, blood thinners, and some pain meds. Knowing your genetic profile can save time and reduce trial-and-error with prescriptions.
How genetics changes treatment choices
If a test shows slow drug metabolism, your doctor might lower the dose or pick a different drug. For example, some antidepressants and antipsychotics have gene-linked dose adjustments. The same idea applies to cancer drugs and newer targeted therapies — they only work if the tumor has certain genetic markers. That’s why genetic testing is routine in many oncology clinics.
Genetics also explains why two people on the same med can have very different experiences. One person might get great results, the other might get bad side effects. Tests can spot differences in liver enzymes and transport proteins that drive those outcomes. When tests exist, they give real, actionable choices.
Practical steps: testing, privacy, and what to ask
Thinking about testing? Start by asking your doctor which tests matter for your condition or meds. Not every drug needs a test. Insurance coverage varies, so check costs up front. Use accredited labs and keep copies of results — they matter for future care.
Privacy is real. Genetic data can feel personal. Ask how your results are stored, who can access them, and whether the lab shares data for research. Most clinics follow strong rules, but it’s okay to ask for written policies.
Gene therapy and advanced genetic editing are moving fast, but most patients won’t need these yet. Current, practical uses of genetics are about better prescribing, cancer matching, and diagnosing inherited conditions. If you read headlines about “cures,” ask how widely available and proven a new approach is before getting excited.
Want something actionable? If you take a chronic medication that isn’t working or causes side effects, bring up pharmacogenomic testing with your clinician. If you have a strong family history of a disease, ask about targeted genetic screening. Small steps can change treatment for the better.
Explore our related articles below to see examples, guides, and simple how-tos — from drug alternatives to thyroid and diabetes options where genetics plays a role. Use genetics as a practical tool, not a buzzword. It can make your treatment safer and more effective.
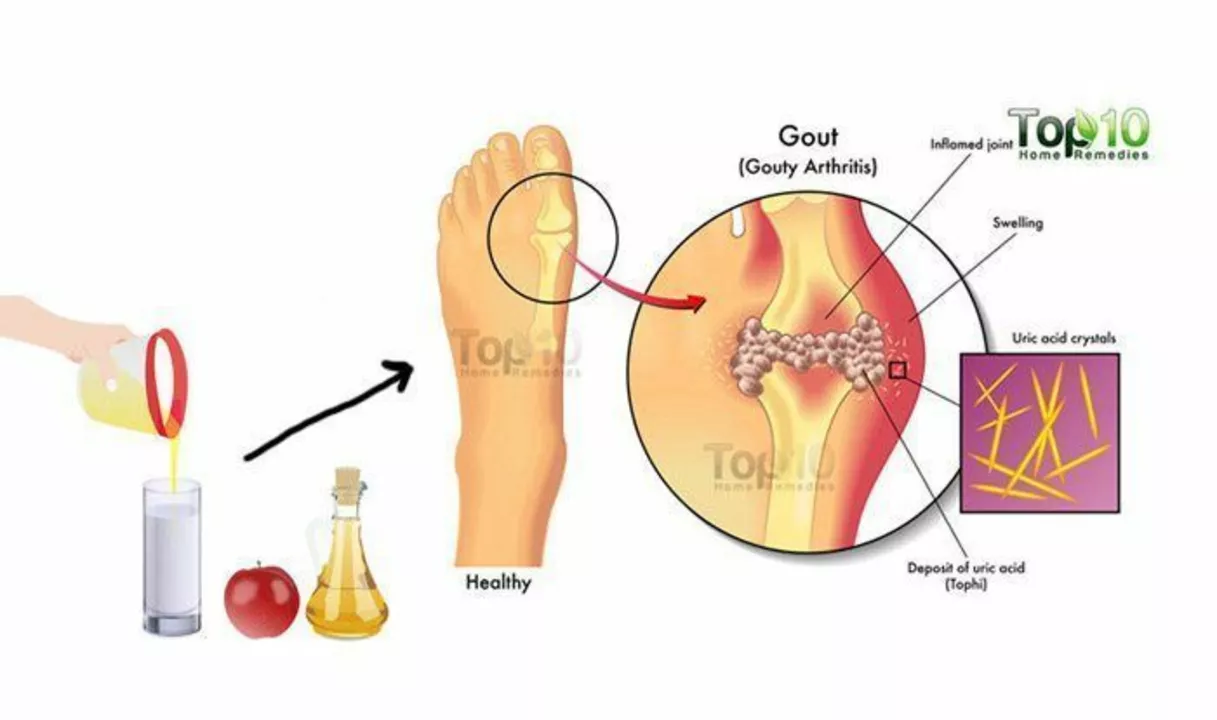
The Role of Genetics in Gouty Arthritis: Are You at Risk?
As a blogger, I recently delved into the fascinating topic of genetics and its role in gouty arthritis. What I discovered is that genetics plays a significant part in determining an individual's risk for developing this painful condition. In fact, certain genes have been identified that are associated with an increased risk for gout. This means that if you have a family history of gout, you may be more susceptible to developing it yourself. It's crucial to be aware of this genetic link and take preventive measures to minimize your risk of experiencing the discomfort of gouty arthritis.
- Drug Information (75)
- Health and Wellness (60)
- Pharmacy Information (28)
- Medical Conditions (24)
- Supplements (5)
- Diabetes (4)
- Travel Health (3)
- Mental Health (3)
- Heart Health (2)
- Parenting (2)
-
OTC Constipation Remedies: Fiber, Stool Softeners, and Laxatives Explained
17 Mar 2026 -
How to Manage Medication Storage in Shared Living Spaces
1 Jan 2026 -
Experience the Healing Wonders of Artemisia Herba-Alba: Your New Go-To Dietary Supplement
12 Jun 2023 -
How the US Government Regulates Generic Drug Prices
4 Feb 2026 -
VA Generic Coverage: How Veterans Affairs Formularies Control Prescription Costs and Access
7 Jan 2026

2.06.23
Alistair Mukondiwa
11